Prepared by Dr Mohd Roslan bin Haron
Consultant Clinical Oncologist
Gleneagles Medini Hospital
Definition of cancer almost always will include phrases like “uncontrolled
proliferation of cells in the body that can invade surrounding tissues and spread to distant structures and
organs…” Whatever the definition maybe, clinically
or in the ‘laymen’s’ term, cancer has always been associated with death, misery and suffering in
the minds of the newly diagnosed patients.
The diagnosis of hypertension or a cardiovascular disease or diabetes (which are more
common than cancer) is usually well accepted by the newly diagnosed without the fear of death, misery or suffering
lingering in our minds. Little do we know that CVDs
diseases are the leading cause of death; and little do we realise that diabetes can be a life-long disease requiring
intense treatment and self-control. Let alone the misery leading to its complication.
The Department of Statistics Malaysia in its Press Release on the Statistics on Causes of
Death, Malaysia, 2018 revealed that Cancer lies 5th amongst the causes of death in Malaysia with
2.4-2.7% in the male population.
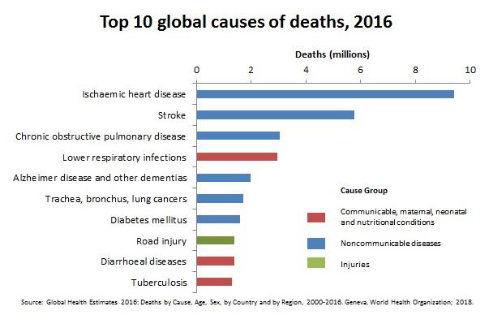
Death related/due to cardiovascular disease (mainly ischaemic heart disease) was the main
cause of death at 15.3-16.0%. These findings tally with the report from WHO 2018 Global Health Estimates of 2016
stating that the number one cause of death globally
is related to cardiovascular events rather than cancer. And yet, the stigma of death, misery and suffering somehow
is only and always attached to the cancer illness.
Minimising the cancer stigma
As much as we do not want to attach any other illnesses with this awful attitude, our
state of mind seemed to have been set to perceive such, most often out of ignorance, lack of understanding and fear.
The success of any particular treatment of cancer depends on many variables. Apart from
the clinical features of the disease (the main factor), factors like the attitude of the patient as well as the next
of kin or caregiver are also important in ensuring
the success of any treatment that has been planned for the patient. It is only upon completion of the
treatment successfully; can the predicted outcome of treatment be made more meaningful.
Understanding cancer prognosis
It is therefore very important that patient’s are given proper understanding of
their disease and the treatment that will be given in order to eradicate if not to minimize the stigma that cancer
is “death, misery and suffering”. Only
then, can treatment be given optimally and successfully, a very important key towards cancer cure.
Another factor that plays an important role in cancer prognosis is the stage of
detection. It is a well-known fact that the earlier cancer is detected, the higher are the chances of
successful treatment. Various developments in the fields
of genetic profiling have now enabled medical practitioners to identify those at risk and make recommendations for
regular check-ups accordingly, to catch the disease (if it happens to show up) at the beginning stage.
Understanding cancer treatment
Optimal cancer treatment is often linked to efficient clinical
management of the disease. Most importantly, in an effort to achieve efficacy and efficiency of any
particular treatment, a guideline of the overall treatment policy for each
individual patient should be outlined from the word go. With this approach, an individual with cancer will and
should be managed by a team of multi-disciplinary cancer care providers. For example, in the Hospital setting, the
Tumour Board Committee
should be the centre of the patients medical and clinical management with inputs from related healthcare providers.
With the many changes and development in the arena of cancer treatment over the past few
decades, there is always something that can be given as treatment to all patients. Treatment is usually given with
the aim of cure for the majority of patients but
sometimes this may not be possible, especially with advanced disease. In which instance, palliative treatment is
usually the intent of treatment.
Whereas the holistic treatment of cancer should actually begin at home, the choices for
treatment at the hospital depends on many factors like the staging of the cancer, its histological features and
surely, the patients consent to treatment.
There are many different kinds of treatment that can be given including surgery,
chemotherapy, radiotherapy, targeted and immune therapy and many others. In almost all cases, treatment is usually a
combination of two or more of the above treatment modalities.
Treatment is usually tailored to suit each individual patient differently, depending on their cancers and is never
the same for all patients.
Cancer treatment usually involves delivery of repeated treatments scheduling and can be a
long and tiring journey. Treatment compliance and adherence to scheduled hospital visits are some areas of concern
that can affect the completion of treatment. The
main reason to this is patient’s inability to tolerate the various side effects of treatment.
Importance of psychosocial support
Although many different methods of intervention are available to minimise those side
effects, many other non-clinical factors can also help to improve treatment compliance. This includes psychosocial
support and encouragement especially from the next
of kin and other family members. Support groups also work wonderfully to provide the necessary motivation as well as
also share success stories. These are also perhaps the best places to get first-hand knowledge and tips on common
issues like how
to successfully manage radiation treatment or chemotherapy.
Affordability in cancer treatment
Another very important issue is that of financial competence. Cancer treatment is none
but expensive and can be a burden for all. Provision of affordable and modern cancer treatment facilities is indeed
a big challenge for both the government as well
as the private enterprise. Compulsory health care insurance is one method of trying to solve this, but its
implications need to be identified and addressed correctly before it can be a success.
It is also very heartening to note that the integration of robotics and artificial
intelligence (AI) in surgeries have enhanced the accuracy and speed at which surgeons can work. Various procedures
are now minimally invasive and require a shorter recovery
which is a big relief to patients. Robotics has also improved the effectiveness with which tumours can be removed,
and that too without harming the healthy surrounding tissues.
Further, chemotherapy and its side effects have always been an overwhelming topic for
patients. Many prefer living with cancer than undergoing the side effects of chemotherapy. However, advancements in
the field of cancer pharmacotherapy have made it
possible for patients to take chemo orally, without the need to stay in a hospital for intravenous administration.
New generation chemo medications do not necessarily kill the cancerous cells. Instead, they work by altering the
tumorous tissue’s
DNA to enable the body’s immune system to get rid of it. Overall, the approach is much safer and does not have
the side effects of traditional chemotherapy. (Source: Biospectrum India)
There are many areas that still need to be addressed and many more will appear as we move
on with time for betterment of cancer treatment. Remember, there is always something that can be done for all
patients that have been diagnosed with cancer and it
is surely NOT the end of the world; as ‘cancer’ is just a word, not a sentence and definitely,
definitely NOT a death sentence.


6fddc7d0-20f4-4624-b0a2-4e1017fc3b63.jpg?sfvrsn=404d305_6)
cdd280d3-fa9c-4039-b020-f062e04d69fe.jpg?sfvrsn=79f2453f_6)